Does tPA have side effects
 Mia Lopez
Mia Lopez Complications of TPA Because TPA is a powerful blood thinner, the main side effect is bleeding. Bleeding is a serious complication that can result in a hemorrhagic stroke, which is often more serious than an ischemic stroke.
What are the symptoms of tPA?
- Hemorrhage (bleeding) affecting the brain: Causes headaches, weakness, confusion, loss of consciousness, seizures.
- Hemorrhage of the digestive system: Causes blood in the stool or stomach pain.
- Severe blood loss: Causes lightheadedness, low blood pressure, loss of consciousness.
Why does tPA cause intracranial hemorrhage?
The risk of hemorrhage is increased because tPA triggers plasmin activation, which degrades cross-linked fibrin into fibrin split products and reversal agents. Reperfusion injury and breakdown of the blood-brain barrier may also contribute to the risk of symptomatic intracranial hemorrhage.
What is the pharmacological effect of tissue plasminogen activator tPA )?
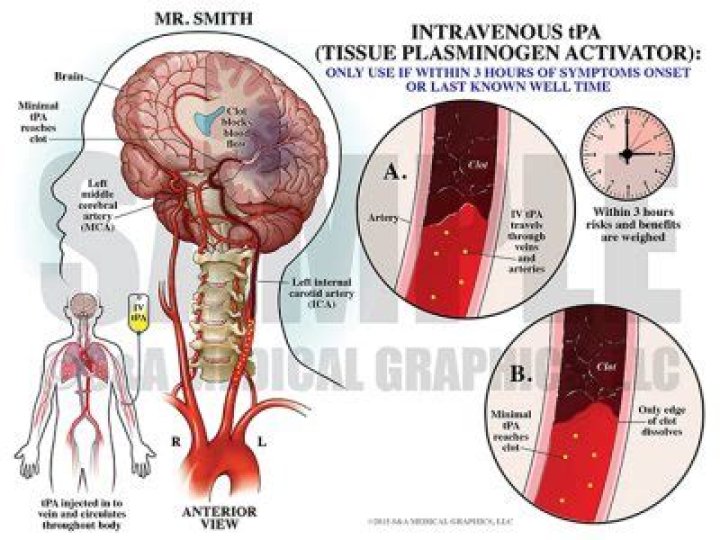
Tissue plasminogen activator (tPA) is an intravenous medicine given for ischemic stroke – a stroke caused by a blood clot – that can dissolve the stroke-causing clot. Studies show that people who receive tPA within 3 hours – up to 4.5 hours in some patients – have better and more complete recoveries.What are the side effects of clopidogrel?
- excessive tiredness.
- headache.
- dizziness.
- nausea.
- vomiting.
- stomach pain.
- diarrhea.
- nosebleed.
Which one of the following is a plasminogen activator?
There are two main plasminogen activators: urokinase (uPA) and tissue plasminogen activator (tPA). Tissue plasminogen activators are used to treat medical conditions related to blood clotting including embolic or thrombotic stroke, myocardial infarction, and pulmonary embolism.
What are the side effects of heparin?
- Abdominal or stomach pain or swelling.
- back pain or backaches.
- bleeding from the gums when brushing teeth.
- blood in the urine.
- coughing up blood.
- headaches, severe or continuing.
- heavy bleeding or oozing from cuts or wounds.
- joint pain, stiffness, or swelling.
What is plasminogen activity?
Plasminogen Activity – The precursor of plasmin is plasminogen, plasmin lyses fibrin clots. Activity is increased in pregnancy and as an acute phase reactant. Rare hereditary deficiency of plasminogen predisposes to venous thrombosis. Low activity is associated with DIC, liver disease, and increased risk of thrombosis.What activates tissue plasminogen activator?
The activation of plasminogen to plasmin in blood is catalyzed by t-PA secreted from endothelial cells. Fibrin provides binding sites for both plasminogen and t-PA, thereby optimizing contact between them.
What are the side effects of alteplase?- nausea,
- vomiting,
- low blood pressure (hypotension),
- dizziness,
- mild fever, or.
- allergic reactions (swelling, rash, hives).
Which of the following is the most likely clinical use of the enzyme tPA tissue plasminogen activator )?
tPA is used in some cases of diseases that feature blood clots, such as pulmonary embolism, myocardial infarction, and stroke, in a medical treatment called thrombolysis. The most common use is for ischemic stroke.
What is tissue plasminogen system?
Tissue plasminogen activator (tPA) is a serine protease that catalyzes the conversion of plasminogen (plg) to plasmin, which in turn functions to degrade extracellular matrix proteins in the central nervous system. The tPA-plasmin system plays a role in synaptic plasticity and remodeling.
When do bleeding complications occur after tPA?
Most SICH hemorrhages will occur within the first 24 hours after receiving IV r-tPA, with the bulk of fatal hemorrhages occurring within the first 12 hours.
Does tPA cause headaches?
In our study, patients treated with IV tPA had a headache incidence of 32.6%, which is consistent with previous reports of headache incidence in AIS patients (8%–43%).
What is tPA in stroke treatment?
An IV injection of recombinant tissue plasminogen activator (tPA) — also called alteplase (Activase) — is the gold standard treatment for ischemic stroke. An injection of tPA is usually given through a vein in the arm with the first three hours. Sometimes, tPA can be given up to 4.5 hours after stroke symptoms started.
What are the most common side effects of Plavix?
- nosebleeds, pale skin, easy bruising, purple spots under your skin or in your mouth;
- jaundice (yellowing of your skin or eyes);
- fast heartbeats, shortness of breath;
- headache, fever, weakness, feeling tired;
- little or no urination;
- a seizure;
What is famotidine used for?
Famotidine is used to treat stomach ulcers (gastric and duodenal), erosive esophagitis (heartburn or acid indigestion), and gastroesophageal reflux disease (GERD). GERD is a condition where the acid in the stomach washes back up into the esophagus.
What are the side effects for Tamsulosin?
- sleepiness.
- difficulty falling asleep or staying asleep.
- weakness.
- back pain.
- diarrhea.
- runny or stuffy nose.
- pain or pressure in the face.
What's the most common side effect of heparin?
The more common side effects of this drug include: bruising more easily. bleeding that takes longer to stop. irritation, pain, redness, or sores at the injection site.
What's the most common side effect of heparin Weegy?
Common side effects may include: unusual bleeding or bruising; uncontrolled bleeding; allergic reactions; or.
What is the most serious potential side effect of heparin is?
- skin warmth or discoloration;
- chest pain, irregular heartbeats;
- shortness of breath, dizziness, anxiety, sweating;
- any unusual bleeding or bruising;
- severe pain or swelling in your stomach, lower back, or groin;
What activates plasminogen to plasmin?
Plasminogen is converted to plasmin by cleavage at the Arg561-Val562 peptide bond by tissue-type or urokinase-type plasminogen activator (tPA and uPA, respectively). Activation of plasminogen by tPA is the major pathway that leads to lysis of fibrin clots.
What products are formed as the result of plasmin activation?
After being generated, plasmin digests fibrin in a pattern that produces a collection of degradation products, including fragment X, fragment Y, and the core fragments, fragments D and E.
When is plasminogen activated?
Plasminogen activation is tied to activation of the coagulation system and can involve secretion of physiologic PAs (“extrinsic activation”). It has been suggested that kallikrein, factor XIa, and factor XIIa, in the presence of HMWK, can directly activate plasminogen.
Where is TPA synthesized?
TPA is synthesized in vascular endothelial cells and released into the circulation, where its half-life is approximately 3 minutes and its plasma concentration averages 5 ng/mL.
What triggers plasminogen?
The most physiologically active plasminogen activator is tissue plasminogen activator (tPA), its production and secretion are predominantly from endothelial cells. [1] The endothelial release of tPA gets triggered by numerous local stimuli, including shear stress, thrombin activity, histamine, and bradykinin.
What is a recombinant tissue plasminogen activator?
Listen to pronunciation. (ree-KOM-bih-nunt TIH-shoo plaz-MIN-oh-jen AK-tih-vay-ter) A form of tissue plasminogen activator that is made in the laboratory. It helps dissolve blood clots and is used to treat heart attacks, strokes, and clots in the lungs.
What is the plasminogen test?
The method is an automated chromogenic assay in which an excess of streptokinase (SK) in the presence of fibrinogen is added to sample plasma containing plasminogen. A plasminogen-streptokinase complex is formed.
Is plasminogen a plasma protein?
Plasminogen is an abundant plasma protein that exists in various zymogenic forms. Plasmin, the proteolytically active form of plasminogen, is known for its essential role in fibrinolysis.
What is congenital plasminogen deficiency?
Congenital plasminogen deficiency is a disorder that results in inflamed growths on the mucous membranes, which are the moist tissues that line body openings such as the eyelids and the inside of the mouth. Development of the growths are usually triggered by infections or injury, but they may also occur spontaneously …
What are the side effects of epoetin alfa?
- Bone or joint pain.
- general feeling of tiredness or weakness.
- heartburn or belching.
- itching or stinging at the injection site.
- loss of strength or energy.
- muscle aches or weakness.
- skin pain.
- stomach discomfort, upset, pain, or swelling.