What does cuffed trach mean
 Leah Mitchell
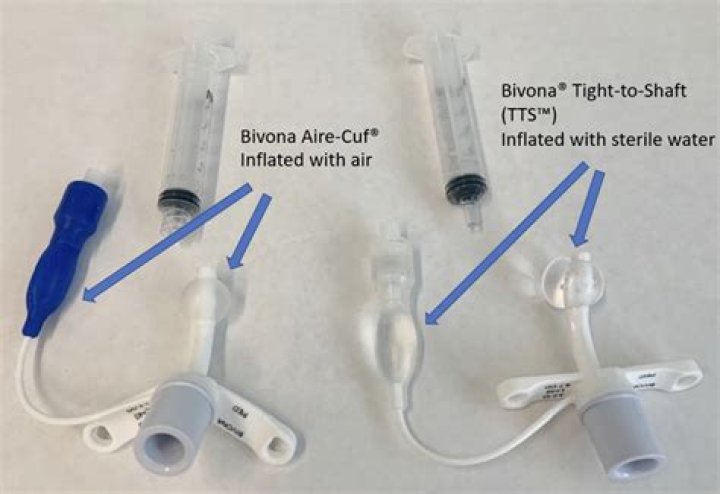
Leah Mitchell What is a cuffed tracheostomy tube? A tracheostomy tube may be either “cuffed” or “cuffless (uncuffed).” A cuffed tracheostomy tubes has a balloon-like feature at the distal end of the tube. There are three main types of cuffs: low-pressure cuffs, low-volume cuffs and foam-filled cuffs.
What's the difference between cuffed and uncuffed Trach?
Tracheostomy tubes can be cuffed or uncuffed. Uncuffed tubes allow airway clearance but provide no protection from aspiration. Cuffed tracheostomy tubes allow secretion clearance and offer some protection from aspiration, and positive-pressure ventilation can be more effectively applied when the cuff is inflated.
Can a patient talk with a cuffed trach?
Cuffed tubes usually are used in acute care and for mechanically ventilated patients. When the cuff is inflated, air must pass through the tracheostomy tube to enter and exit the lungs. Because air no longer passes over the vocal cords, speech isn’t possible.
Why are some Trach cuffed?
Cuffed tubes allow positive pressure ventilation and prevent aspiration. If the cuff is not necessary for those reasons, it should not be used because it irritates the trachea and provokes and trap secretions, even when deflated.Can you swallow with a cuffed trach?
If your tracheostomy tube has a cuff, the speech therapist or provider will ensure the cuff is deflated during meal times. This will make it easier to swallow. If you have a speaking valve, you may use it while you eat. It will make it easier to swallow.
When should a trach be cuffed?
A cuff is necessary when a patient is on a mechanical ventilator. Inflating the cuff during mechanical ventilation makes sure that air is entering the lungs and not escaping through the nose and mouth. The cuff also prevents aspiration of saliva in patients who have trouble swallowing.
When would you use an uncuffed tracheostomy?
An uncuffed tube is suitable for a patient in the recovery phase of critical illness who has returned from intensive care and may still require chest physiotherapy, suction via the trachea and airway support.
How do you clean a cuffed tracheostomy tube?
Steps to clean a tracheostomy tube Add clean tap water and mild soap. Be sure the tube, obturator, and strap are covered by water. Soak them for a few minutes to loosen any secretions. Clean the tube and other parts using pipe cleaners and gauze sponges.What complication can present from having a cuffed tracheostomy tube?
- Increased risk of tracheal injury, including mucosal injury, stenosis, granulomas, and more;
- Diminished ability to use the upper airway, leading to disuse atrophy over time; and.
The Passy-Muir speaking valve is commonly used to help patients speak more normally. This one-way valve attaches to the outside opening of the tracheostomy tube and allows air to pass into the tracheostomy, but not out through it. The valve opens when the patient breathes in.
Article first time published onHow does PMV help swallowing?
Improves Swallow & May Reduce Aspiration The bias-closed position Valve restores the patient to a more normal closed system which facilitates increased pharyngeal and laryngeal sensation and restores positive subglottic air pressure.
How do I know if my trach cuff is inflated?
Inject 0.5 cc of air at a time until air cannot be felt or heard escaping from the nose or mouth (usually 5 to 8 cc). If the patient is able to talk, the cuff is not inflated adequately (air is vibrating the vocal cords). Small pilot balloon on outside of the tube will inflate, indicating that the cuff is inflated.
How does Passy Muir work?
When placed on the hub of the tracheostomy tube or in-line with the ventilator circuit, the Passy Muir® Valve redirects air flow through the vocal folds, mouth and nose enabling voice and improved communication.
What happens if a tracheostomy cuff is deflated?
When the cuff is deflated, some airflow is reestablished through the upper airway. There is movement of airflow both through the tracheostomy tube as well as through the upper airway. This increases the effective airway diameter.
What happens if cuff pressure is too high?
High cuff pressures can result in complications ranging from sore throat and hoarseness to tracheal stenosis, necrosis, and even rupture. In such cases, the postulated causative factor is diminished blood flow to tracheal mucosa due to excessive cuff pressure on the tracheal wall.
Which tracheostomy complication is the most serious?
Obstruction. Obstruction of tracheostomy tube was a common complication. The most frequent cause of obstruction was plugging of the tracheostomy tube with a crust or mucous plug. These plugs can also be aspirated and lead to atelectasis or lung abscess.
How long does it take for a tracheostomy hole to close?
Healing of the tracheostomy wound: when the tracheostomy tube is removed the wound left should heal over within 1-2 weeks.
How much air should be in a trach cuff?
How to Inflate Cuff. Measure 5 to 10 mL of air into syringe to inflate cuff. If using a neonatal or pediatric trach, draw 5 ml air into syringe. If using an adult trach, draw 10 mL air into syringe.
How do you place a PMV?
Place PMV on trach hub: keep one hand on the trach flange to maintain trach tube position in airway, without creating pressure to the trachea or discomfort for the patient. 5. Give valve ¼ turn clockwise. Do not place PMV on forcefully, as this will make it difficult to remove.
What is PMV medical term?
The Passy-Muir Tracheostomy & Ventilator Swallowing & Speaking Valve is often referred to the shortened name of Passy-Muir Valve or by the acronym PMV or PMSV. PMV is the term for prolonged mechanical ventilation and therefore if an acronym is used in a medical setting PMSV is preferred to reduce confusion.
What is a PMV trial?
∎ Passy-Muir Valve (PMV) enables patient to vocalize without use of fingers or trach. caps. ∎ PMV is a “no leak” one-way speaking valve that allows air in through the trach on. inhalation and blocks air escape through the trach on exhalation.
Can you sleep with a Passy Muir valve?
The PMV is formally indicated for wake time use only; however, beneficial effects may be hastened if patients were also permitted to sleep with the PMV in place. To date, the use during sleep has not been reported.
How often should the Passy Muir valve be replaced?
The PMV should last at least two months if you care for it properly. If the PMV becomes sticky, noisy or vibrates during use, it is time to replace it.
Does Passy Muir valve humidify?
HMEs retain heat and moisture of the patient’s expired air to warm and humidified the next inspired breath. NOTE: An HME will be ineffective when a speaking valve is in place.